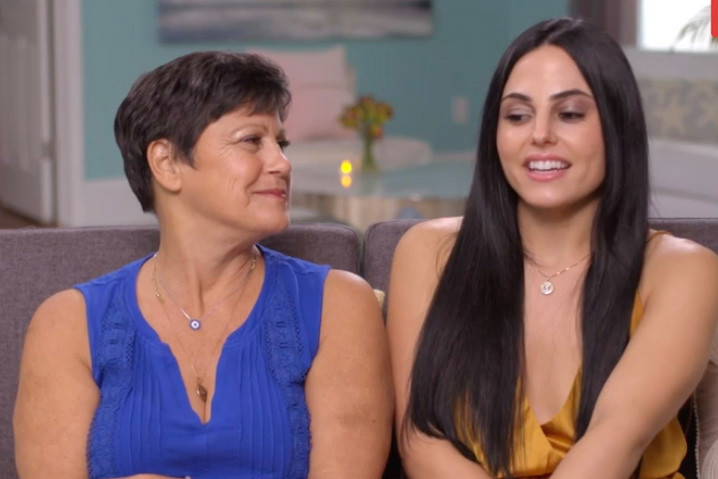Top News
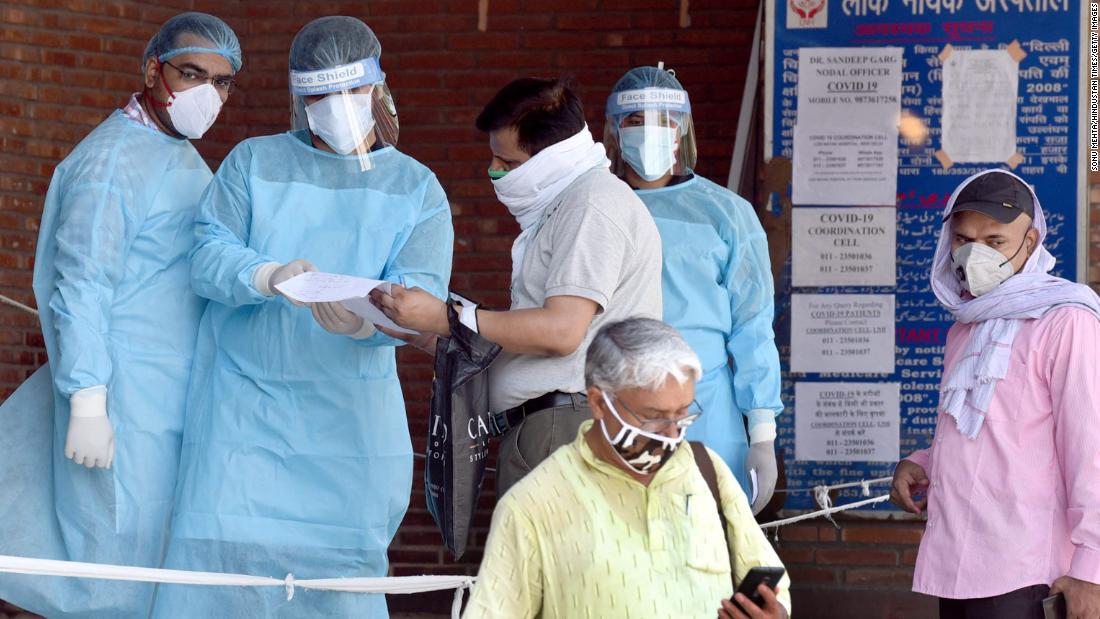
When Delhi became the capital of the Indian coronavirus, the hospital struggled to overcome it
A day later, an online report confirmed that he was positive.
“We are not panicking,” said Singh’s son-in-law, Mandeep. “Because we know the reason for the fever, we think we might be able to overcome it.”
But when Singh’s condition worsened, his family found it impossible to find a hospital that would treat him, because the city’s health care system was bent under increasing epidemic pressure.
Mandeep Singh said three private hospitals told the family that they did not have a bed, even though an application made by the Delhi government indicated they had availability. Others did not even take phone calls 68 years old, including those he tested.
Finally, Lakhjeet Singh went to Lok Nayak Jai Prakash Narayan (LNJP) – the biggest government hospital in Delhi. Before they departed on the 30-minute trip to the hospital, Mandeep Singh said government applications showed the hospital had 1,100 beds available.
But when they arrived, Mandeep Singh claimed his father-in-law was rejected by medical staff, even though the government hospital in Delhi was legally bound not to reject emergency patients. Medics say there are no free beds.
“It is very unlikely that 1,100 beds will be occupied by the time we get to the LNJP hospital,” Mandeep Singh said.
Outside the hospital, old Singh fainted. His family forced him inside, where 10 minutes later a doctor examined him and declared him dead on arrival.
In a statement, LNJP expressed condolences to the Singh family and denied that he was refused entry. The hospital said he was examined by a doctor and died on arrival.
On June 4, Lakhjeet Singh’s daughter wrote a short message on Twitter: “She’s not there anymore. The government is disappointing us.”
The highest Covid-19 count in India
When India was locked on March 25, Delhi had recorded only 606 cases of Covid-19 and 10 deaths. When the city first began to loosen lockout restrictions in the third week of May in an effort to revive its economy, the numbers began to increase – and on June 8, there were more than 40,000 cases.
Sisodia warns that Delhi would need 80,000 more hospital beds in such a scenario.
Dr. Arvind Kumar, chairman of the Chest and Lung Transplant Center at Sir Ganga Ram Hospital in Delhi and founder of the LungCare Foundation, said the situation in Delhi was “frightening.”
“At present, the numbers are increasing very fast and the problem with this infectious disease is that as the infected group increases in the community, the number of cross infections that occur from the infected group also increases and multiplies,” he said.
At a press conference on Monday, Delhi Chief Minister Arvind Kejriwal said around 23,000 new Covid-19 cases had been reported in the city in the past 10 days. Last week, Delhi Health Minister Satyendar Jain was stated positive.
About 55% of Covid-19 cases are active in isolation at home, officials say, but the rest need medical attention.
As cases escalated and people rushed to look for hospital beds, in early June the city government launched the Delhi Corona Application, which displays real-time information about the availability of beds in government and private hospitals. Hospitals enter information into the platform, and government officials cross-check these figures.
Kejriwal said the application, which is updated twice a day, would help bridge the information gap regarding bed status and could be used to register complaints against hospitals that refuse to accept infected patients.
But with applications that show free hospital beds in many facilities, it seems that the problem is not just providing more beds: hospitals also need staff to take care of them.
Lack of medical personnel
Shahana Chanda, 34, was taken to at least five hospitals in early June, according to her uncle, Shahid Siddiqui, a local politician.
Although the hospital application said beds were available, his family said he was repeatedly refused from the facility, until finally being treated at the famous central government hospital at Delhi-Safdarjung Hospital.
Chanda was tested for Covid-19 upon admission and was given a bed – but after that, her family said she was ignored.
“There is no one to look after him,” said Siddiqui. “No medication was given. He was left alone, only oxygen was given.”
Chanda died on June 7. Siddiqui said she was releasing her oxygen supply to walk to the bathroom on the ward, where she fainted. “When he fell, no one came to help him. His brother had to take him back to bed. When the doctors examined him, they said he was no longer,” Siddiqui said.
Safdarjung Hospital said in a statement that Chanda was in critical condition when treated and that his family had wasted important time taking him to a different hospital. The hospital said Chanda was initially tested negative for the corona virus.
The persecution does not end there, said Siddiqui.
“When he died, the brother was asked to put it in a bag, sew it and bring it to the morgue, and put it there. There was no one there to help them,” he said.
Safdarjung Hospital told CNN that they would not respond to the allegations.
One TV report shows a man lying on the ground naked in a ward, with an elderly unconscious on a nearby bed. There is no medical staff ready to help.
Parv Mittal, president of the Resident Doctors Association at LNJP Hospital, said the facility was overwhelmed on the day of recording.
“There is a shortage of medical and household staff. Doctors and nurses take rounds but are too much of a burden. Many have contracted the infection due to long working hours. The situation is much better now,” he said. “More and more domestic workers are being employed and CCTV cameras have been set up to monitor sick patients.”
The Supreme Court asked Delhi officials to increase the number of beds in the entire state and to “provide the right infrastructure and staff” for Covid-19 patients, calling the conditions “sad” and “inappropriate.”
Action taken
Indian Home Minister Amit Shah reviewed the situation in Delhi after the Supreme Court’s scathing report, and then set a series of standard operating procedures after talks with the Delhi government.
Among other measures, the cost of isolation beds in private hospitals has been significantly reduced – while Delhi’s testing rate, which the Supreme Court considers low, has been increased from an average of 5,000 tests every day to 18,000, according to Chief Minister Kejriwal.
Officials say another 20,000 Covid-19 beds will be added there next week. This includes a large spiritual center that will be converted into a specialist hospital with 10,000 beds – expected to be the largest Covid-19 center in the world – on Friday.
In addition, 500 old train trainers, with a total of 8,000 beds, have been designated as centers of isolation for mild cases.
But experts still doubt that Delhi has enough manpower to operate additional facilities.
Kumar, from Sir Ganga Ram Hospital, said front-line workers were exhausted and afraid of getting infected by the virus.
“We don’t have enough manpower to run even our own hospital today,” he said. “We fight with nurses every day. They want to resign, they want to leave. The resident doctor disappeared overnight … People don’t want to do the work here … There are labor problems in every hospital.”

General internet buff. Hardcore music maven. Typical foodaholic. Friendly student.
Top News
Portuguese historical films will premiere on 29 December.

Method Media Bermuda will present the documentary FABRIC: Portuguese History in Bermuda on Thursday, December 29 at the Underwater Research Institute of Bermuda.
A spokesperson said: “Method Media is proud to bring Bermuda Fabric: Portugal History to Bermuda for its 5th and 6th showing at the Bermuda Underwater Observatory. In November and December 2019, Cloth: A Portuguese Story in Bermuda had four sold-out screenings. Now that Bermuda has reopened after the pandemic, it’s time to bring the film back for at least two screenings.
“There are tickets Ptix.bm For $ 20 – sessions at 15:30 and 18:00. Both screenings will be followed by a short Q&A session.
Director and producer Milton Raboso says, “FABRIC is a definitive account of the Portuguese community in Bermuda and its 151 years of history, but it also places Bermuda, Acors and Portugal in the world history and the events that have fueled those 151 years.
“It took more than 10 years to implement FABRIC. The film was supported by the Minister of Culture, the Government of the Azores and private donors.
“Bermuda Media Method [MMB] Created in 2011 by producer Milton Raposo. MMB has created content for a wide range of clients: Bermuda’s new hospital renovation, reinsurance, travel campaigns, international sports and more. MMB pays special attention to artistic, cultural and historical content.
More about
Model: Everybody, Entertainment, Movies/Movies, History, News

Proud web evangelist. Travel ninja. Creator. Freelance food nerd. Passionate bacon fanatic.
Top News
CRISTANO RONALDO CAN MAKE UP A GIANT IN CARIOCA AND PORTUGUESE TECHNICIAN SAYS ‘There will be room’

News
This is a fact or event of journalistic interest. This may be new or recent information. This also applies to the novelty of an already known situation.
Article
Mostly original text. Expresses the opinion of the author, but not necessarily the opinion of the newspaper. It can be written by journalists or specialists from different fields.
Investigative
A report that contains unknown facts or episodes with a pronounced denunciatory content. This requires special methods and resources.
Content commerce
Editorial content that offers the reader conditions for making purchases.
Analysis
This is the interpretation of the news, taking into account information that goes beyond the facts told. It uses data, brings events and scenario forecasts, as well as past contexts.
Editorial
Analytical text translating the official position of the vehicle in relation to the facts covered.
Sponsored
This is an institutional article on a topic of interest to the company sponsoring the report.
fact checking
Content that confirms the accuracy and authenticity of the disclosed information or facts.
Context
This is an article that brings subsidies, historical data and relevant information to help understand a fact or news.
special
An exciting report that details the various aspects and developments of this topic. It brings data, statistics, historical context, as well as stories of characters that are affected by or directly related to the topic in question.
Interview
A subject-specific approach in which the subject is presented in a question and answer format. Another way to publish interviews is through threads, where the interviewee’s answer is reproduced in quotation marks.
Criticism
A text with detailed analysis and opinions on products, services and works of art in a wide variety of fields such as literature, music, film and visual arts.

Proud web evangelist. Travel ninja. Creator. Freelance food nerd. Passionate bacon fanatic.
Top News
Maestro de Braga is the first Portuguese in the National Symphony Orchestra of Cuba.

Maestro Filipe Cunha, Artistic Director of the Philharmonic Orchestra of Braga, has been invited to conduct the Cuban National Symphony Orchestra, as announced today.
According to a statement sent by O MINHO, “he will be the first Portuguese conductor to conduct this orchestra in its entire history.”
In addition to this orchestra, the maestro will also work with the Lyceo Mozarteum de la Habana Symphony Orchestra.
The concerts will take place on 4 and 12 March 2023 at the National Theater of Cuba in Havana.
In the words of the maestro, quoted in the statement, “these will be very beautiful concerts with difficult but very complex pieces” and therefore he feels “very motivated”.
From the very beginning, Rachmaninoff’s Piano Concerto No. 2 will be performed by an Italian pianist (Luigi Borzillo), whom the maestro wants to bring to Portugal later this year. In the same concert, Mendelshon’s First Symphony will be performed.
Then, at the second concert, in the company of the Mexican clarinetist Angel Zedillo, he will perform the Louis Sfora Concerto No. 2. In this concert, the maestro also conducts Tchaikovsky’s Fifth Symphony.
“This is an international recognition of my work. An invitation that I accept with humility and great responsibility. I was surprised to learn that I would be the first Portuguese member of the Cuban National Symphony Orchestra. This is a very great honor,” the maestro said in a statement.
“I take with me the name of the city of Braga and Portugal with all the responsibility that goes with it, and I hope to do a good job there, leaving a good image and putting on great concerts. These will be very special concerts because, in addition to performing pieces that I love, especially Rachmaninov and Tchaikovsky, I will be directing two wonderful soloists who are also my friends. It will be very beautiful,” concludes Filipe Cunha.

Proud web evangelist. Travel ninja. Creator. Freelance food nerd. Passionate bacon fanatic.
-
World3 years ago
The Gabby Petito case. Brian Landry set up camp with his family after his girlfriend disappeared
-
Top News4 years ago
Tristan Thompson reacts to Khloé Kardashian’s new appearance
-
Top News4 years ago
TLC ‘sMothered’ recap: ‘Party curled up,’ boyfriend problem
-
Top News4 years ago
Alex Cooper hosts a solo podcast
-
Top News4 years ago
2021 Ford Bronco price: Here’s how much the 2-door and 4-door cost
-
Tech4 years ago
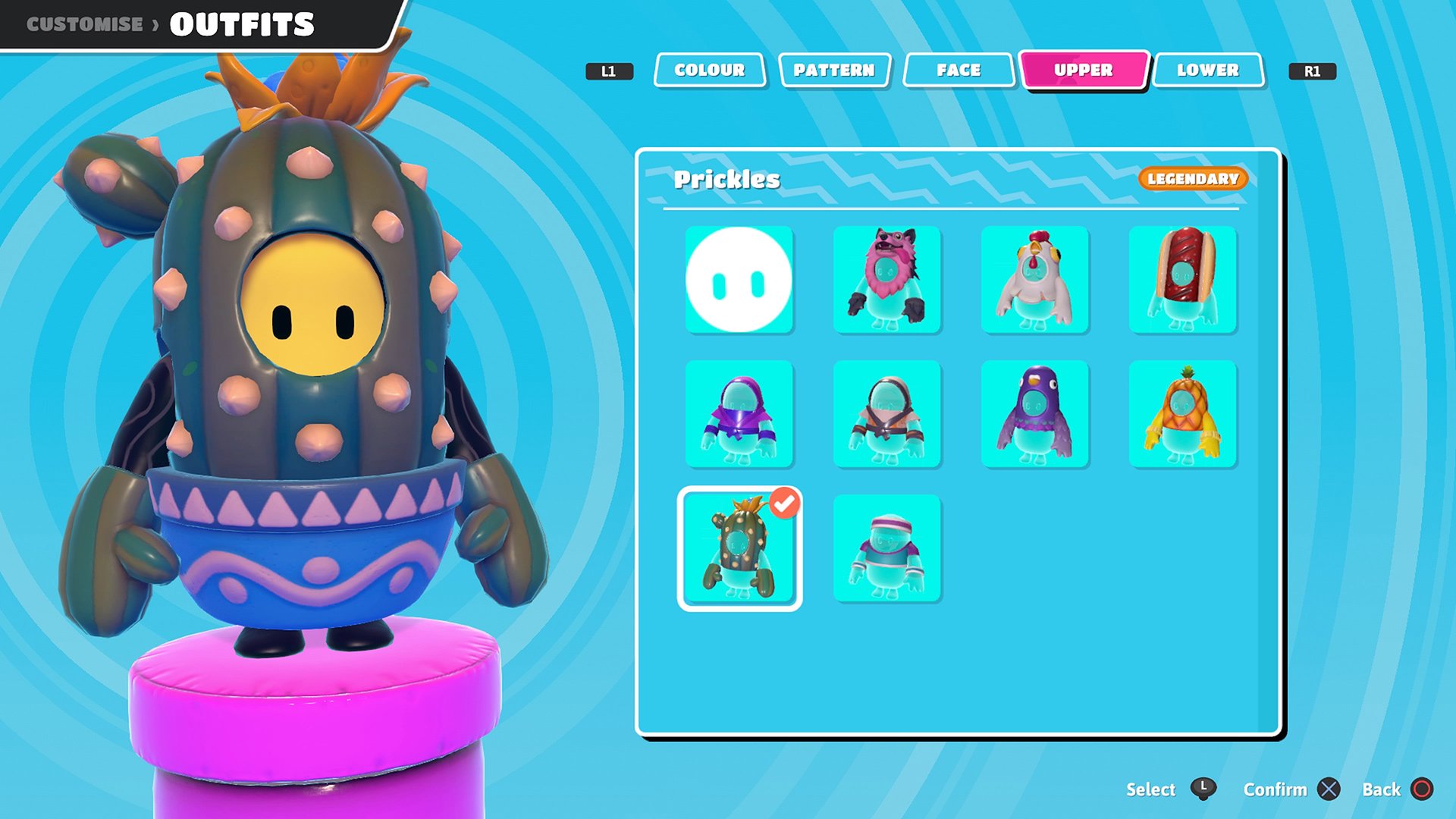
Fall Guys is supplying out a legendary costume and Kudos as an apology present
-
Top News4 years ago
Chiara de Blasio was ‘very cold’ during the arrest of the protest: witness
-
Top News4 years ago
How to Watch Yellowstone Season 3, Episode 2 Live Online